|
By Emma Meyers
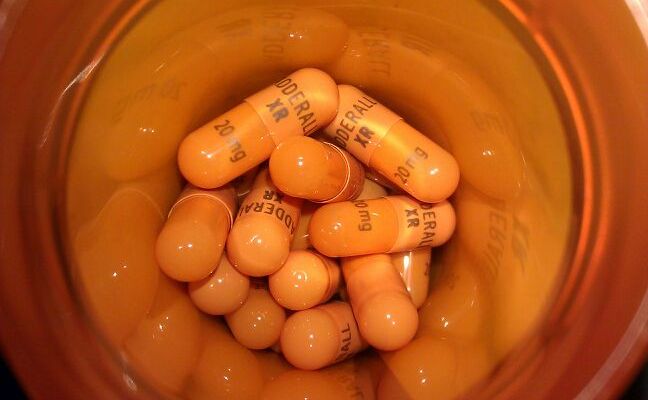
Why the sudden media spotlight on adderall? Seriously, it seems like it’s been all over the news lately. In the past six months, the New York Timeshas published a slew of occasionally terrifying articles about adderall, ritalin, and other attention-enhancing drugs. People condemn it and praise it, scoff at it and crave it, but I’m mostly just left wondering, “Isn’t adderall made of amphetamine…like methamphetamine? Why are we not all zombie meth addicts killing each other for pills in the library?” So, I set out to figure out what goes on in your brain when you pop an Addy and settle in for a long night in Butler. But first, I know this is a contentious topic (just read some of those Times articles…then read some of the comments on those articles), so I’d like to say right off the bat: this is neither a condemnation nor a condoning of the use of stimulants in adults or children, prescribed or not. It is merely a look into the psychopharmacology of the drug so that we can all understand what the media’s favorite pill does in our brains. Adderall is a mix of two stereoisomers of amphetamine, a stimulant related to the recreational drugs methamphetamine and MDMA, or ecstasy. Adderall’s chemical structure is close to those of the catecholamine family of neurotransmitters and hormones, which includes epinephrine, norepinephrine, and dopamine. This similarity confers Adderall’s neurotropic effects by allowing it to mimic the action of these brain chemicals. Normally, catecholamines function in areas of the brain that control emotion and arousal, among other things. Dopamine, for instance, plays a prominent role in reward and pleasure pathways, and norepinephrine modulates the sympathetic nervous system, which drives our “fight or flight” response. The hormone epinephrine (probably better known as adrenaline) also has a part in the sympathetic catecholaminergic response, and contributes to the rush we feel when we are nervous or excited. As a catecholamine agonist, taking Adderall recreates these sensations by binding to the receptors for dopamine and norepinephrine in the brain and epinephrine in the adrenal gland. Additionally, it blocks the activity of the transporters that remove catecholamines from the synapse to end the response, and actually allows for some reverse transport of endogenous catecholamines out of the neuron into the synapse so that they can bind their receptors as well. Effectively, Adderall floods the brain with amp-up, feel-good chemicals, leaving us feeling alert, euphoric, and ready for anything. Like any drug, though, Adderall comes with a host of side effects and potential dangers. The intense arousal can lead to insomnia and anxiety, which in turn can descend into schizophrenia-like psychosis (as one of those Times articles I mentioned above discusses). Since amphetamines work on the body as well as on the brain, Adderall causes elevated heart rate and increases in blood pressure, which can be bad news for people with pre-existing heart conditions. And, like all other drugs (you name it – alcohol, caffeine, which is actually works by a similar mechanism to amphetamines and which wrote about a while back in CSR), Adderall has the potential to be addictive. A Schedule II controlled substance, it shares its high risk of dependence with the likes of cocaine, opium, oxycodone, and methamphetamine. Given these properties, are A.D.H.D. sufferers and overachieving students alike all unwitting meth users destined to the throws of addiction? Not quite. Though studies have shown that when taken in comparable doses, methamphetamine and Adderall (amphetamine) are effectively identical, there are some differences between the two drugs. For example, it is believed that the additional methyl group on methamphetamine makes it more fat soluble and, therefore, more efficacious. Also, some researchers believe meth may not be as villainous as we make it out to be, so even if the conflation of Adderall and methamphetamine is justified, it is not necessarily a death sentence to occasional and regular amphetamine users. So, whether you swear by Adderall or shudder at the thought of it, at least now you know how it works. Use it. Or don’t. Either way, please try not to end up like him or her. And next time you’re staring straight into the ugly face of another all-nighter and have some choices to make, use science as your guide. Happy studying!
0 Comments
The end of the Devil? Well, the Tasmanian devil that is. Sadly, that might well soon become a reality as a fatal contagious cancer is decimating the population of this marsupial. Found exclusively in Tasmania as their name suggests, devils, scientifically known as Sarcophilus harrisii, are small, primarily nocturnal scavengers with an unusually small amount of genetic diversity in their population.
According to a March 11th report in the Proceedings of the National Academy of Sciences, Cambridge scientists have estimated that over 70% of the Tasmanian devil population has already been killed off by this cancer that continues to rapidly spread across the central and eastern parts of the island. Since these marsupials seem to have no defensive mechanisms against this genetic invader, the fatality rate appears to be an alarming 100%. So what exactly is a contagious cancer? Quite simply, the name tells the full story: a contagious cancer is in fact a type of cancer that can spread among different individuals due to the relatively stable genome of the cancerous cells when they are transmitted. However, this disease is exceeding rare, and only a few organisms (namely dogs, hamsters, and devils) have been documented to suffer from this affliction. In dog populations however, their contagious malignancy, known as Canine Transmissible Venereal Tumor, is usually not fatal, even when no treatment is provided. Why then does Devil Facial Tumor Disease kill pretty much every individual it comes across? At first researchers thought that the answer was in the lack of genetic diversity present in the devil population. However, certain studies involving skin grafts have proven this to not be the case. Devils are usually able to successfully reject foreign cells. Now, progress has been made with the understanding that the difference is one of cancer recognition. While the immune systems of dogs are able to identify the foreign cells and respond to them, the cancer that spreads among Tasmanian devils appears to turn off the production of proteins that typically accomplish identification. As such, the animals cannot recognize the invading cells as being different from their own and therefore produce no immune response. By turning off the major histocompatibility genes (MHC genes), the invading cells become indistinguishable from those of the animal itself. Without a swift human response, the devils from down under don’t stand a chance. The new findings as to how the cancer is able to spread so effectively are, however, a promising step towards dealing with this disease. University of Cambridge geneticist Elizabeth Murchison is hopeful as she explains, “It’s really the first hope that there could be a vaccine or immune therapy.” One possible solution would be to turn on the MHC genes in order to give the immune system a fighting chance against the cancer. Lab studies have already shown that an anti-fungal drug known as Trichostatin A might be able to activate the MHC genes by effecting gene activity. Other positive results have also been achieved with interferon gamma, a genetic chemical that seems to have the same effect. Such studies, however, are very introductory and a possible vaccine or inoculation against the contagious cancer is still long in the making. It remains to be seen whether the Tasmanian Devil populations will have that long to live. By Nate Posey
Speculative fiction has given rise to a breathtaking array of possible futures, ranging from galaxy-spanning empires to tragic self-annihilation. Such timelines diverge from one another through a myriad of technological advances and geopolitical maneuvers, but there is one event which has been accepted as practically inevitable in humanity’s near future: a manned mission to Mars. The red planet has weighed heavily on the imaginations of science fiction writers for decades. While earlier treatments of mankind’s first contact such as Ray Bradbury’s The Martian Chronicles (1950) and Robert A. Heinlein’s Stranger in a Strange Land (1961) exploited the then total ignorance of conditions on Mars to paint fantastic, surreal accounts of advanced Martian civilizations, later works used the extensive findings of remote probes as the basis for a more sober account. My favorite telling is Ben Bova’s Mars, a novel which tracks the expedition of geologist Jamie Waterman and his international crewmates from the heights of Olympus Mons to the depths of the Valles Marineris with Bova’s characteristically impeccable attention to detail. The supreme confidence of speculative fiction writers in this “near future” event has both shaped and been shaped by the corresponding certainty within society’s popular imagination. Only modest extrapolation from the robust advances of the 1960’s in manned spaceflight was required to regard a Mars mission as plausible, if not outright inevitable, in a matter of years. For over a generation, the question has not been if, but when. Here in the year 2013, however, I cannot help but wonder: when indeed? The first practical mission plan for a manned Mars expedition was produced by Werner von Braun in 1948 and published in Collier’s Magazine in 1952. Von Braun, who would go on to design the signature Saturn V rocket of NASA’s Apollo program, remained a key collaborator on subsequent Mars mission proposals as part of Richard Nixon’s Space Task Group. Even as recently as 2004, President George W. Bush reaffirmed the priority of a manned Mars mission as part of his Vision for Space Exploration. As Von Braun’s initial proposals demonstrated, the technology and infrastructure necessary for such a mission has long been at our disposal; all that was needed was the will. And yet, time and time again, this will has failed to materialize. In 2010, President Barack Obama cancelled Bush’s program, scrapping the 2020 deadline for a return to the moon and pushing the long anticipated Mars mission into the ever more nebulous mists of the “near future.” This trend of delay and stagnation has served to cool the expectations of even diehard enthusiasts of the final frontier, and for some such as astrophysicist J. Richard Gott, it has even raised that most terrible of specters: the question of not when, but if. In his book Time Travel in Einstein’s Universe: The Physical Possibilities of Travel through Time, Gott describes the current epoch of manned spaceflight as a precious window of opportunity, a window that may be closing fast. He recounts the chilling story of the black Taj Mahal, a mausoleum which was to be constructed across the river from the existing Taj Mahal as a mirror image of sorts. Although Shah Jahan had ample resources on hand to undertake the project in 1653, he delayed. Five years later, he was deposed by his son Aurangzeb, and to this day the white Taj Mahal stands alone. Of course, even now, nothing stands in the way of the completion of this breathtaking marvel, but the necessary will has long since withered; the opportunity has been forever lost. Gott argues that a similar fate may await man’s oft-envisioned rendezvous with the red planet, and what now seems so inevitable may well be regarded by future generations as a mere historical curiosity, an opportunity lost in time. By Ian MacArthur
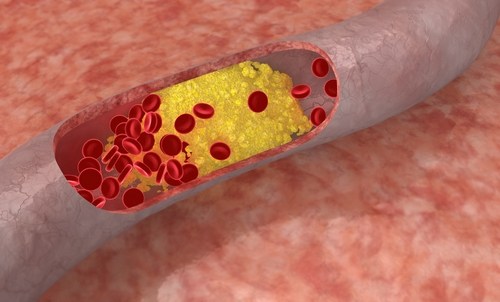
Cholesterol has long been vilified by health professionals as a primary contributor to heart disease. Now, after over sixty years of research, Fred Kummerow of the University of Illinois is challenging this view. Decades of probing the biochemistry of heart disease has led Kummerow to identify oxidized cholesterols and other oxidized lipids as the molecules responsible for the calcification of arteries and lessened blood flow of patients suffering from heart ailments. Oxidized cholesterols, referred to as oxysterols, share a common carbon structure with cholesterol but contain various additional oxygen-containing functional groups. The research process that led Kummerow to reach his conclusion about oxysterols began with a finding that the arteries of patients with heart disease contained elevated levels of sphingomyelin, a phospholipid component of the cell membrane. Comparing the arterial compositions of newborn babies with patients that had undergone bypass surgery, Kummerow found that while newborn arteries contained 10% sphingomyelin and 50% phosphatidylcholine, another phospholipid membrane component, the arteries of bypass patients contained up to 40% sphingomyelin and 27% phosphatidylcholine. Years of additional research then led to the finding that elevated cellular oxysterol levels contribute to the conversion of phosphatidylcholine to sphingomyelin. Arterial calcification in action – when the buildup of calcium from sphingomyelin and calcium ions blocks the flow of blood in blood vessels.Sphingomyelin has since been implicated as a major player in the calcification of arteries. When the phospholipid interacts with ions in blood, it develops a negative charge. Positively charged calcium ions are then drawn towards the negatively charged arterial walls where they amass and constrict blood flow. Oxysterols, then, can be said to facilitate arterial calcification by elevating sphingomyelin levels. Aiding in arterial calcium buildup is not the only way that oxidized lipids contribute to heart disease, Kummerow claims. Additionally, oxidized low density lipoprotein (LDL), erroneously stigmatized as the unhealthy variety of cholesterol, has been linked to the production of thromboxane, a lipid involved in the aggregation of platelets to form blood clots. Further, oxidized LDL may interact with arterial walls to form hazardous lesions. The combined effect that oxidized fats have on calcification and blood clot formation make them one of the most important groups of compounds involved in heart disease. What, then, is the biological significance of cholesterol? Far from causing heart disease, cholesterol has been demonstrated to function as an antioxidant, a substance that inhibits oxidation. In fact, it is believed that cholesterol plays a role in preventing the oxidation of LDL, thereby halting the production of thromboxane and the formation of blood clots. Furthermore, cholesterol is involved in the maintenance of cell membranes, intercellular transport, membrane permeability, and hormone production. While some cholesterol is naturally oxidized enzymatically by the body, the process of frying food produces enough oxysterol to have a deleterious effect on cardiovascular health. Exposure of cholesterol to light, oxygen, and high heat during the frying process gives rise to a host of oxysterols and other oxidized fats that may cause great harm when ingested. Therefore, eating foods high in cholesterol is not necessarily damaging to heart health. However, careful attention to the preparation of such foods should be paid by cardiovascular conscious individuals so as to avoid the ravages of oxysterols, the true culprits behind heart disease. |
Categories
All
Archives
April 2024
|