|
By Alexander Bernstein
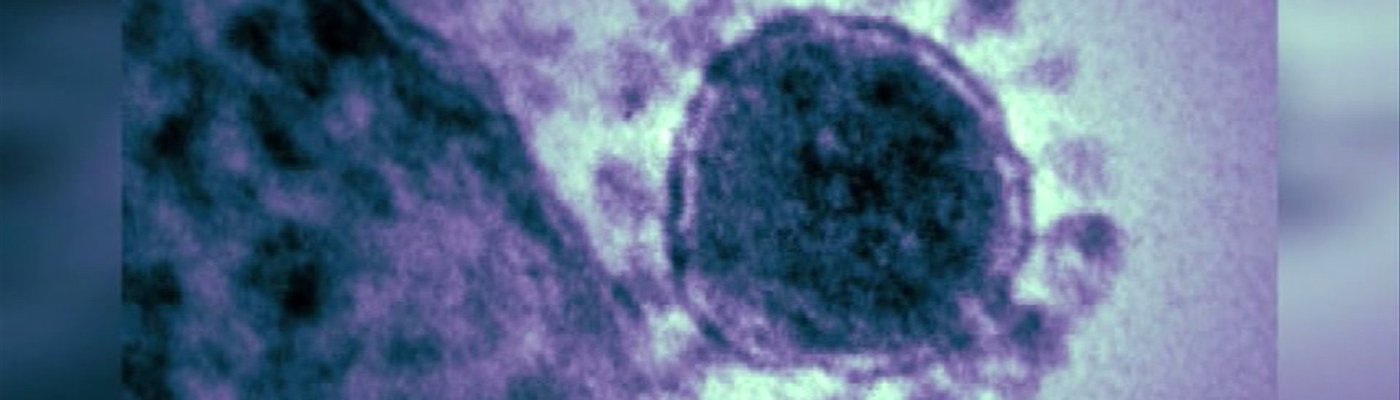
First reported in Saudi Arabia in 2012, Middle East Respiratory Syndrome (MERS) is a coronavirus-caused respiratory illness that has claimed over a 100 lives in Saudia Arabia and has a deadly fatality rate of around 40%. Caused by a virus called MERS-CoV, this illness has since spread to 6 countries near the Arabian peninsula. With patients suffering from fairly generic symptoms such as cough, fever, and shortness of breath, MERS is often compared to the SARS epidemic, which infected over 8,000 people in Asia in 2013. Some of the most notable differences, however, include transmissibility and fatality rate. While MERS is more deadly (40% versus 10% fatality rate), it does not appear to have the same infectious capacity. As such, the disease has primarily been confined to the Middle East. Such is no longer the case. Several weeks ago, as per a report from the Associated Press in New York, the first case of MERS in the United States was confirmed. As might be expected, the afflicted individual had recently returned from a trip to Saudi Arabia, where he had been in Riyadh as a healthcare worker. Flying from Riyadh to London to Chicago and then boarding a bus for Indiana, the man ended up in an Indiana hospital emergency room on April 27th. Although the man is in a stable condition at the Indiana hospital as per a report from Dr. Anne Schuchat, the director of respiratory diseases at the CDC, there are many concerns regarding possible transmission of the disease during the man’s travels. With a typical five-day incubation period for MERS and the patient’s checking in at the hospital on April 27th, experts are still uncertain if he may have infected other individuals. Reporting as a spokesman for the CDC, Tom Skinner explains that although plane tickets can be tracked to determine who the infected man sat next to on his two flights, the “bus ride may be a challenge” since tickets aren’t recorded and monitored in the same way. This particular likely-bat-originated coronavirus hasn’t been found to rapidly spread from person to person. However, localized outbreaks have occurred in hospitals and families where multiple healthcare workers have worked in close proximity to an infected patient. While symptoms can be treated, no cure exists, and potential antibody virus-blocking treatments are still in the early stages of development. The identification of antibodies that attack the particular coronavirus does mark legitimate progress. As per a Harvard led group study, two separate antibodies have been found to interact with the surface of the MERS-CoV and prevent the spike shaped viral protein from attaching to human cells. Of further interest is the discovery that mutations allowing the virus to partially escape the antibodies also appear to result in impaired ability to replicate. Yet, despite the identification of these two antibodies, labeled as MERS-4 and MERS-27, which appear to demonstrate a synergistic effect, researchers are still far from a potential treatment. As Dr. Wayne Marasco, a leading researcher in the Harvard study explains, so far, progress on the matter is only nearing animal testing, with the lack of ideal animal models providing further hindrance to drug development.
0 Comments
Leave a Reply. |
Categories
All
Archives
April 2024
|