|
By Alice Sardarian
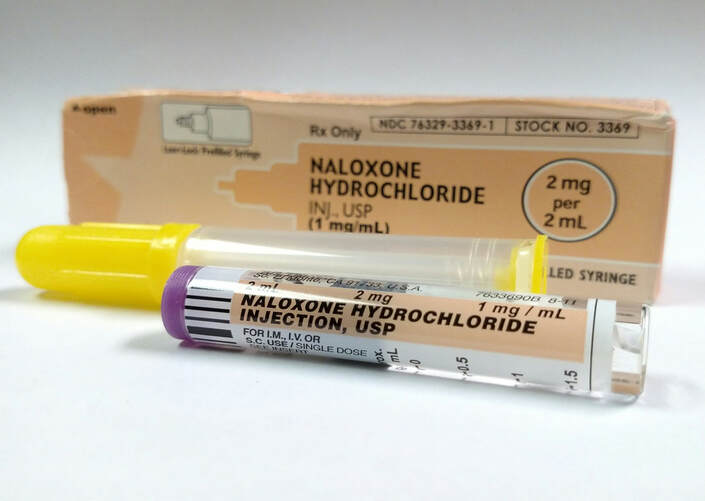
One may be familiar with the red flowers of the delicate poppy plant adorning coats and wreaths on Armistice day, otherwise known as Remembrance day. Most, however, are not familiar with another poppy that has made extensive contributions to the pharmaceutical industry and, unfortunately, has also become a major global health threat. The Papaver somniferum, or opium poppy, is the natural source of opiates. The plant, originally native to the Eastern Mediterranean, is now cultivated all over the world. Afghanistan is the largest producer of opium poppy and opiates: in 2017, the nation produced 9,000 metric tons of opium, which accounted for about two thirds of the global area of illicit opium poppy cultivation in 2016—an area about the size of 427,000 football fields combined. Most of the opiates flooding United States markets, however, originate from South American countries, like Colombia and Mexico. Opioids are composed of three main psychoactive ingredients: morphine, codeine, and thebaine. Common opiates are derived from these main ingredients. For example, heroin is an ester that is formed from morphine. Other opioids are synthetically engineered and significantly more potent, such as fentanyl. Opioids work by binding to opioid receptors in the brain, activating G protein-coupled receptors, and ultimately resulting in a cascade of dopamine. The reception of the dopamine neurotransmitter allows the user to experience pain relief, euphoria, lethargy, and sedation. These are the intended effects of the drugs’ short term use. However, repeated, long-term use of opioids diminishes the sensitivity of opioid receptors. Users, then, require higher doses of the drugs in order to achieve the pain relief and pleasure acquired from their original doses. The physiological dependence and addiction that arise from this continuous need to activate the brain’s reward system has prompted a global health crisis like no other. Opioids are highly addictive, easily accessible, and frequently prescribed. Under these conditions, opioids have become the most abused drugs in the world. The 2015 the World Drug Report indicated an 11% increase in opioid seizures worldwide. Deaths due to opioid overdoses in the United States tally more than 115 individuals per day and continue to increase every year. These deaths pose, for the US alone, an economic burden of over $78.5 billion a year. In order to combat and to address the opioid overdose crisis, authorities have rallied for the inclusion of civilians in the global healing process. For example, Dr. Jerome Adams, the US surgeon general, recently recommended that more Americans, in all walks of life, carry naloxone, a life saving drug easily administered to reverse frequently fatal opioid overdoses. Naloxone administration was previously limited to hospital settings, and a trained medical provider was required to deliver the drug in its syringe form. Today, naloxone is available in a quick and easily inhalable format, under the brand name Narcan. The drug blocks the opioid receptors and, in just two minutes, restores the victim’s failing respiratory capacity. Narcan administration may cause the victim to experience extensive nausea and vomiting, but these are side effects that pale in comparison to the drug’s life saving benefits. Narcan is now available at major pharmacies and is covered by most insurance programs. Anyone can easily visit a naloxone distributor in the vicinity and acquire the life-saving drug. New York City has implemented numerous programs in an attempt to combat its opioid epidemic. About three New Yorkers die every day as a result of an opioid overdose, a number that is three times the city’s murder rate. In March 2017, Mayor Bill de Blasio started the HealingNYC initiative in an effort to accelerate a city-wide response. A primary component of the program is the “Save a Life, Carry Naloxone” campaign. Signs depicting ordinary, citizen heroes are scattered all over the city, above subway entrances and across billboards. They highlight the powerful, life-saving actions of neighbors, family members, and even strangers. New Yorkers are saving New Yorkers. With simple instructions, a non-medically trained, ordinary New Yorker, can reach out to a potential overdose victim and administer the life saving naloxone. Simply put, more individuals can help save the lives of those who may lack access to medical professionals, are disenfranchised, or are simply afraid of authorities. Although the quick and effective treatment of overdoses is essential to saving lives, it is equally important to prevent the overdoses from occurring. Fentanyl is a synthetic opioid that is about 100 times stronger than morphine, and is responsible for 70% of overdose deaths. It is often found in illicit drugs, added by dealers unbeknownst to users. Fortunately, a $1 test strip developed by a Canadian company can help detect the presence of Fentanyl in tainted drug supplies. By targeting illicit drug sources and removing more dangerous products from the drug market, opioid overdoses could be drastically reduced. In addition to preventing excessive Fentanyl exposure, it is paramount to replace or at least minimize opiate prescriptions, which would reduce the risk of developing an opioid dependence. This has been quite difficult, as opioid manufacturers have heavily promoted their products and provided monetary incentives to physicians who prescribe these pain killers. From 2014 to 2016, the pharmaceutical industry, as a whole, spent more than $102 million lobbying members of Congress to prevent the Drug Enforcement Administration from regulating the industry. When physicians and lawmakers receive incentives to keep opioids readily available and to prevent better pain management practices, it is difficult to curtail the prescription of opiates, and the consequent drug dependency and patient addiction that stems from it. Some positive change is taking place to counter the profit-based trend of over prescribed opiates. Dr. Alexis LaPietra of St. Joseph Hospital, NJ, has devised the ALTO program to begin the replacement of frequent opiate prescriptions. The ALTO program outlines alternatives to opiates in the treatment of various medical conditions. To address musculoskeletal pain, for example, instead of opiates, Dr. LaPietra recommends acetaminophen, ibuprofen, muscle relaxants, and trigger point injections. These treatments are effective at relieving pain, while circumventing the excessive distribution of and use of opiates. Since the implementation of the ALTO program in 2016, the Emergency Department at St. Joseph’s has reported a 50% decrease in opiate use and prescriptions, a change that illuminates the efficacy and potential success of alternative pain management approaches. While physicians like Dr. LaPietra are beginning to change the trajectory of this epidemic by not only questioning their practices, but also by drastically changing their treatment strategies, conscientious, educated citizens are also raising awareness and taking further actions against this crisis. Carrying naloxone, emergency medical responders, police officers, librarians, and community members, acting under the Good Samaritan Law, have come together to help save more lives. Today, tragic fatalities from opioid overdoses touch many American lives. This public health emergency is of an epic magnitude, and impacts people from all walks of life. Hence, there is an urgent need to address it on many levels, using multiple strategies and approaches. In order to combat and to eradicate the epidemic, local and nationwide entities must come together to create change on all fronts. These strategies must include and not be limited to: prevention education, decreasing the prescription of opiates, strengthening legislation, weakening big pharmaceutical lobbying, and, most importantly, providing drug users with the support, intervention, and tools necessary to keep them safe and alive. Alice Sardarian is a sophomore at Barnard College majoring in Physiological & Organismal Biology. She is managing editor for the Columbia Science Review.
0 Comments
Leave a Reply. |
Categories
All
Archives
April 2024
|