|
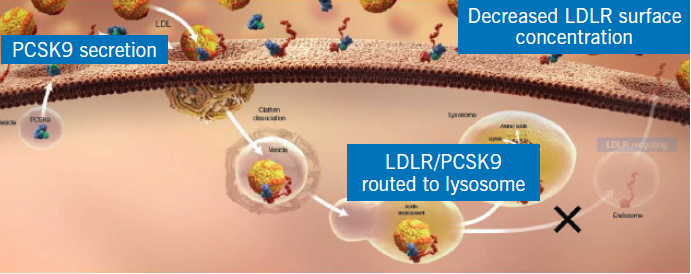
By Tiago Palmisano Edited By Bryce Harlan One reason I love biology is that despite centuries of research and discovery, we are continuously gaining new insight into the machinations of the human body. Even today our understanding of medicine is expanding as biotechnology and pharmaceutical companies strive to develop more sophisticated strategies for combating disease. In this article I want to discuss two potentially game-changing advances in medicine. PCSK9 Inhibitors The PCSK9 protein binds to the LDL-receptor on the surface of liver cells. This causes the LDL-receptor to be degraded, which prevents the uptake of LDL cholesterol from the blood. The PCSK9 inhibitors stop this process. (via The British Journal of Cardiology)
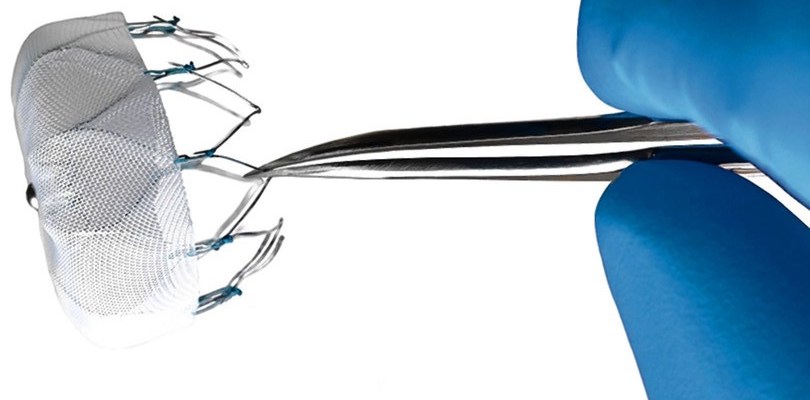
In order to understand the significance of PCSK9 inhibitors, it is first necessary to understand the physiology of cholesterol. Cholesterol is a modified steroid that serves an essential role in all animals. Among other things, cholesterol is required to maintain the integrity of cell membranes and to synthesize hormones and bile acids. This important molecule does not travel in the body independently, but rather is carried through the bloodstream in capsules known as lipoproteins. Two types of lipoproteins exist in the human body, known as HDL (high-density lipoprotein) and LDL (low-density lipoprotein). Although cholesterol is a crucial component of bodily functions, elevated concentrations (known as high cholesterol) are problematic. Specifically, a high level of LDL can result in coronary heart disease, which in turn may lead to a heart attack. Typical treatment of this condition involves a class of drugs known as statins, which lower LDL levels by inhibiting an enzyme necessary for the production of cholesterol. Various statins are available on the pharmaceutical market, accounting for billions of dollars in sales. However, a new class of drugs known as PCSK9 inhibitors may soon give statins a run for their money. PCSK9 is a naturally occurring protein that binds to the receptor for LDL cholesterol on liver cells. When LDL cholesterol binds to this receptor, it is taken up by the liver cell and removed from the blood. However, the PCSK9 protein can bind to the LDL-receptor and initiate breakdown, preventing the receptor from taking up cholesterol. Put simply, the PCSK9 protein prevents the removal of LDL from the blood. And this is where the brilliance of pharmaceutical advancement comes into play. The newly developed PCSK9 inhibitors are monoclonal antibodies that do exactly what they say – they bind to PCSK9 and inhibit its normal function. If PCSK9 cannot attach to the LDL-receptor, then more receptors are available to take up LDL and the levels of cholesterol in the blood decrease significantly. Currently, the Food and Drug Administration has approved two PCSK9 inhibitors for use in the United States (alirocumab and evolocumab). Research has demonstrated that PCSK9 inhibitors are much more effective than statins at lowering LDL levels. For example, one study found that PCSK9 inhibitors lower LDL levels by approximately 60% in patients already taking a statin! Furthermore, PCSK9 inhibitors are given via injection every 2-4 weeks, whereas statins are taken as a daily pill. Such an improvement in efficiency suggests that it is only a matter of time before they replace statins as the go-to prescription for treatment of high cholesterol. WATCHMAN Left Atrial Appendage Closure Device The WATCHMAN device is inserted into the heart via a catheter, and it sits in the left atrial appendage. This prevents blood clots in the left atrial appendage from escaping into the bloodstream and causing a stroke. It is vital to note that drugs are not the only form of modern medical advancement. Large-scale medical devices are also becoming increasingly sophisticated, and the WATCHMAN device is the latest example. As its name suggests, the WATCHMAN closes the left atrial appendage. But what does this mean? Well, the heart is composed of four chambers, two atria and two ventricles. In this case, we are looking at the left atrium in particular. Electrical signaling in your body causes the heart to contract, which pushes blood out of the left atrium and into the left ventricle. For an unknown reason, there is a small pouch (an “appendage”) on the wall of the left atrium. Normally this is not a problem, as the contraction of the heart pushes all of the blood out of this appendage. However, the left atrial appendage becomes an issue if the contractions are abnormal. Coronary heart disease, high blood pressure, and age can all result in atrial fibrillation (AF), a condition in which the electrical signals in the heart fire irregularly. AF disrupts the heart’s contractions and allows blood to collect in the left atrial appendage, since effective transfer of blood to the left ventricle does not occur. Over time this collected blood can clot, and these clots can result in a stroke if they are pumped out of the heart. If AF occurs, then the left atrial appendage becomes a problem. The typical method for preventing stroke in patients with AF is warfarin, a blood thinner that inhibits the formation of clots. However, since the left atrial appendage is not actually necessary, Boston Scientific has developed an interesting way to prevent strokes in patients with AF. The WATCHMAN device is a net-like implant that is designed to sit in the left atrial appendage. This device is delivered to the heart via a catheter, and once in place it expands to fill the appendage. By effectively closing off the left atrial appendage, the WATCHMAN device prevents potential clots from escaping, decreasing the risk of a stroke. The major benefit of this alternative treatment is that warfarin, the typical treatment, has numerous adverse side effects. For example, blood thinners such as warfarin can lead to excessive bleeding, known as hemorrhage. The WATCHMAN solves the issue of stroke risk without thinning the blood, and therefore many doctors may begin to view this new device as the safer and preferable option.
0 Comments
Leave a Reply. |
Categories
All
Archives
April 2024
|